This is another great project on personality assessment in active duty military personnel who underwent a neuropsych evaluation with Pat Armistead-Jehle. Also, the work of Tristan (Picture above; lab postbac) and Sarah McCracken (check the lab members webpage) were fantastic. I’ll summarize our work / findings.
Previous research on the PAI has examined response patterns in those with recent brain injuries. While some studies (Kennedy et al., 2015; Velikonja et al., 2010) have identified a four-group solution (low/non-symptomatic, High, Moderate, and Somatic Distress), others (Demakis et al., 2007) have suggested a three-group solution (high distress, manic/high energy, and externalizing groups). Moreover, research has not employed the entire span of PAI scales. The current study sought to address some of these gaps by using LPA to examine response patterns on the PAI in active-duty military personnel with a remote history of brain injury (n = 384).
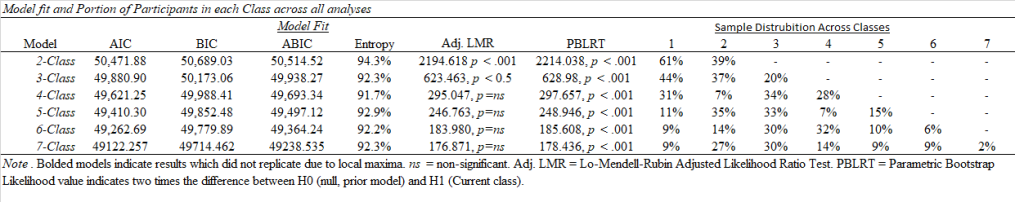
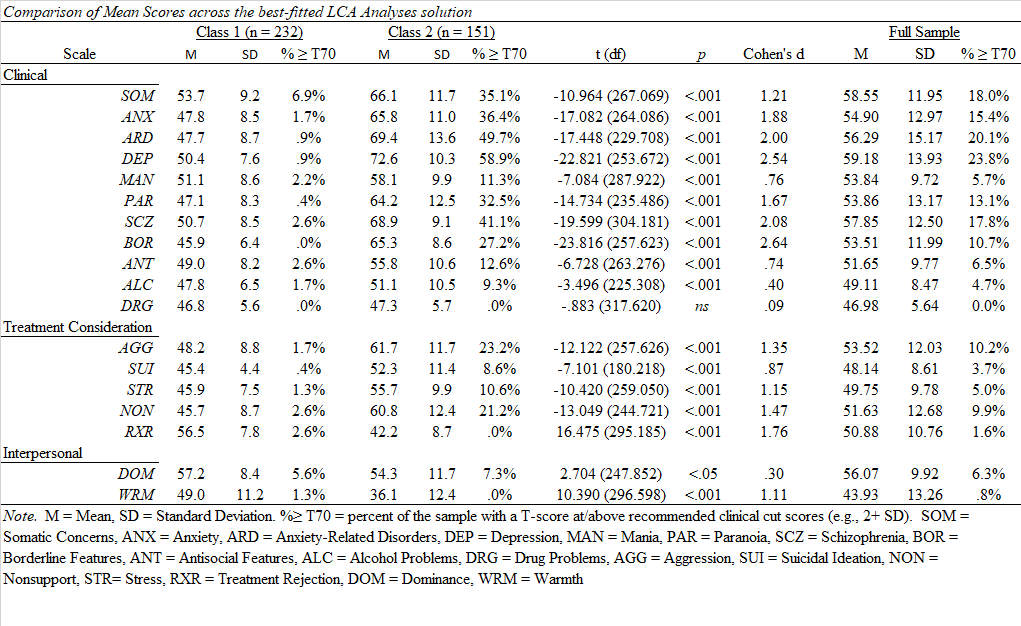
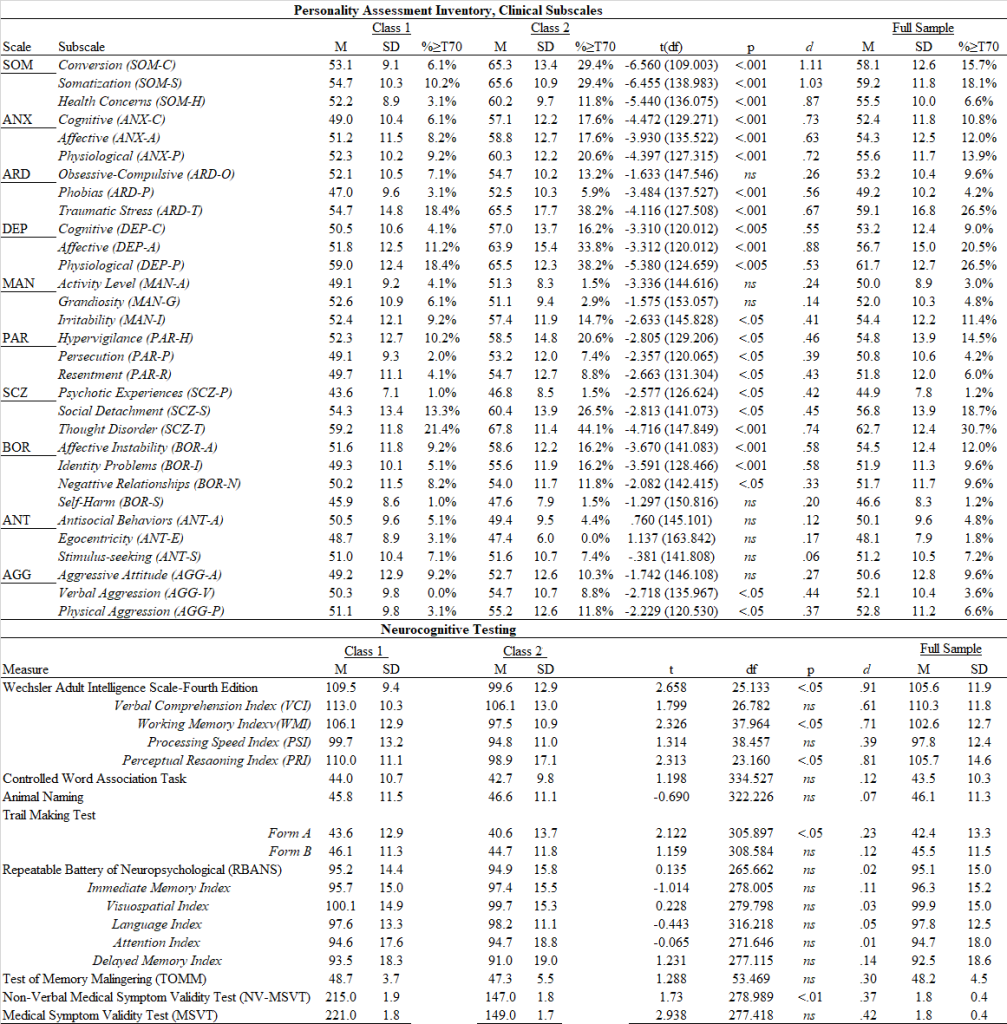
LPA were conducted using the Clinical, Treatment, and Interpersonal Scales because of their non-overlapping item content. The best-fitted model (based on AIC/BIC/SSA-BIC/Entropy & Parsimony/theory-based interpretation) was contrasted across PAI subscales, as well as neuropsychological testing, PVT, and demographic data. Results suggest a 2-class solution (non-symptomatic [59%] and high symptomatic [40%]), with no differentiation between subsets of symptoms (e.g., manic, externalizing, or somatic, per earlier studies). Scale differences reflected generally large effects, particularly for SOM, ANX, ARD, DEP, PAR, SCZ, and BOR (d = 1.07 – 2.50). High symptom groups also evidenced poorer neurocognitive testing and more frequent PVT failure. These findings suggest that previously identified response groups are not evident in active-duty military with a remote history of brain injury. Some tables below to show off some of the results of the poster (Click to download).